Contraception and pregnancy
Contraception and pregnancy are subjects that arise frequently on our helplines. The advice given to acute patients is generally quite different to that given to those with skin porphyrias. But whichever porphyria you have, we have guidance to help you. If in doubt, please contact us and we can put you in touch with a relevant specialist to help.
Contraception in the acute porphyrias
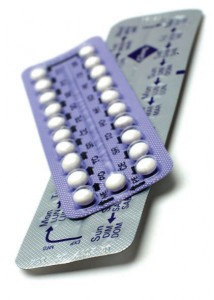 Contraception is often a tricky subject for those with one of the acute porphyrias (AIP, VP, HCP or ALA-D deficiency porphyria).
Contraception is often a tricky subject for those with one of the acute porphyrias (AIP, VP, HCP or ALA-D deficiency porphyria).
Oral contraceptive pills are listed on the UNSAFE drugs list. They are known to provoke attacks of acute porphyria, either alone or by interacting with other factors. The pill, particularly the progestogen element, can trigger acute attacks. However, some women who have inherited one of the acute porphyrias can take the pill without adverse effects. It is not recommended in anyone with active porphyria. Unfortunately, there is no way of knowing how a woman with porphyria will react to the pill. It is a risky option and should never be undertaken lightly. The general advice is to avoid the pill and other hormonal methods of contraception. In particular, injectable and implanted hormonal preparations should never be used as they cannot be removed if an attack starts.
So, now we know what to avoid, what are the alternatives?
The simplest solution is to use a barrier method of contraception. Eg the male or female condom, the diaphragm or the cervical cap. Physical barrier methods can offer effective and acceptable birth control to individuals who use them consistently and correctly. Importantly, the condom is the only method to adequately protect against sexually transmitted infections (STIs) and HIV.
Other contraceptive options include inter-uterine devices (IUD) such as the copper coil or the Mirena coil. The Mirena coil contains a progestogen that has a local action within the uterus and only enters the bloodstream in very small amounts. Experience to date suggests that this sort of device carries an extremely low risk of provoking an acute attack. It is regularly used for patients with active acute porphyria. Copper IUDs especially are not suitable for all women (they can cause heavy periods and stomach cramps), whereas the Mirena coil can alleviate some of these symptoms. Some young women who have not had children may have problems convincing their doctor that it is a good idea.
In terms of emergency contraception, ‘the morning after pill’ contains high doses of progestogen which are dangerous in porphyria! For emergency contraception insertion of an inter-uterine device is the safe alternative.
Overall, it should be possible to take responsible steps to ensure that you have a solution which suits your lifestyle. Talk to your GP or family planning clinic about appropriate options.
Pregnancy in acute porphyria
Research presented at the Porphyrins and Porphyrias conference in Stockholm (2009) included a study by British doctors Joanne Marsden and David Rees, on the outcome of pregnancy in patients with acute porphyria.
Although the sample was relatively small (only 15 women), obstetric complications were few and porphyria related complications were also minor. The report also revealed that a couple of women more severely affected by their porphyria were treated with Haem Arginate during pregnancy. Haem was well tolerated with no adverse effects being observed on the baby (although this is no guarantee that this is safe yet). More research will need to be undertaken to investigate this further.
Although nearly all pregnancies for those with an acute porphyria, i.e. AIP, ADP, VP or HCP, are uneventful, there is a small risk of having an acute attack during or after pregnancy. It is therefore vital that the doctors providing care during pregnancy know that you have an acute porphyria.
Why is there an increased risk of attacks?
Pregnancy is associated with increased levels of hormones such as progesterone, which may aggravate porphyria. However, attacks caused in this way are uncommon.
The major risk is that some of the medications used in pregnancy are unsafe for those with acute porphyria. They could be prescribed by mistake either during the pregnancy or delivery period.
It is important that the SAFE drugs list (download here) is always adhered to. Advice should be sought from a porphyria specialist or the UK Porphyria Medicines Information Service (UKPMIS). UKPMIS can also be contacted by telephone on 029 2074 3877 or 029 2074 2251.
If you have a porphyria specialist, they may liaise with the obstetric team to ensure that your file contains a list of SAFE drug options for each of the circumstances that could occur before, during or after the birth.
Some notable drug points are:
- Safe antibiotics are readily available and can be chosen easily from the SAFE list.
- Vaccines such as whooping cough are safe.
- Prostaglandins given intravaginally are safe, e.g. Oxytocin (Syntocinon®, Pitocin®).
- Ergometrine and ergometrine combinations are dangerous and must be avoided.
- There are many safe opiates, epidurals and general anaesthetics on the SAFE list to choose from.
Download a handy factsheet about pregnancy and porphyria.
What happens if I have an attack during pregnancy?
If an attack occurs during pregnancy, it should be treated promptly and according to your normal protocol.
There is no experimental data to verify the safety of haem arginate use in pregnancy. However, it has been safely administered in pregnant women over recent years, with no ill effects to mother or baby.

